

Safer Sex & Polyamory
Safe sex and STDs are a very real concern for everyone, but especially for those who have multiple sexual partners. When people engage in monogamous relationships, it is assumed that there are no other sexual partners. With high statistics of people admitting to have cheated at least once in their lives, this means that even in monogamous relationships, we are all at risk for sexually transmitted diseases and infections. Even without cheating, many people are actually "serial monogomists", meaning they have several partners over a lifetime, and many STDs can lie dormant for years.
In fact, the latest research shows that HPV is so easily transmitted, that it is showing up in 9 year old girls who have not had sexual contact and HSV (herpes) can be transmitted from an infected parent giving their child a kiss while shedding the virus around their mouth. So even monogamy with only one partner ever is not safe from infections labeled as "STDs" because some infections can be transmitted through non-sexual contact. When people have open and honest sexual relationships, theoretically the people involved at least know what they are risking. It is up to each individual to determine what their risk level is and to set the limits they are willing to take.
First we will start with what the various STDs are with a chart created with the latest information from the Centers for Disease Control and Prevention, the Community Health Services Dept. of Lambton County, the American Social Health Association, and others. You can also keep updated with the latest STD information over at The InnKeeper's Journal - STI Research & Updates.
| STI | Description | Symptoms | Transmitted | Treatment | Complications | Rate of Infection | Condom Effectiveness |
| Bacterial Vaginosis | A condition in women where the normal balance of bacteria in the vagina is disrupted and replaced by an overgrowth of certain bacteria. It is sometimes accompanied by discharge, odor, pain, itching, or burning. | Discharge, odor, pain, itching or burning. | Unclear. Sometimes through sexual contact. | Antibiotics | Can increase a woman's susceptibility to other STD infections, increased susceptibility of infection following surgical procedures, complications during pregnancy. | Most common vaginal infection. | Unknown |
| Chlamydia | Caused by the bacterium, Chlamydia trachomatis, which can damage a woman's reproductive organs. Even though symptoms of chlamydia are usually mild or absent, serious complications that cause irreversible damage, including infertility, can occur "silently" before a woman ever recognizes a problem. Chlamydia also can cause discharge from the penis of an infected man. | Many males and most females have no symptoms. May have burning on urination, discharge, abdominal pain, pain during sex, or females may bleed during or after sex. Symptoms begin 1-3 weeks or longer after contact. | Oral, anal, and vaginal sex; mother to child. | Antibiotics | Women - if untreated: Infertility; infected cervix; pelvic pain; pelvic inflammatory disease; ectopic pregnancy, arthritis. Infants can get pneumonia or become blind. Men - if untreated: Infertility; arthritis; eye infections; urinary infections. | 2.8 million new infections each year. | High |
| Gonorrhea | Caused by a bacterium that can grow and multiply easily in the warm, moist areas of the reproductive tract, including the cervix (opening to the womb), uterus (womb), and fallopian tubes (egg canals) in women, and in the urethra (urine canal) in women and men. The bacterium can also grow in the mouth, throat, eyes, and anus. | May have no symptoms - especially females. May have burning while urinating, and thick yellowish discharge. | Contact with the penis, vagina, mouth, or anus, and from mother to baby through childbirth. Ejaculation does not have to occur for gonorrhea to be transmitted or acquired. | Antibiotics | Can cause PID in females which can lead to sterility. Can cause heart and brain infection. Can cause blindness in infants if infected during birth. | 120.9 infections per 100,000 persons. | High |
| Syphilis | Caused by bacterium. Sores occur mainly on the external genitals, vagina, anus, or in the rectum. Sores also can occur on the lips and in the mouth. The chancre is usually firm, round, small, and painless. It appears at the spot where syphilis entered the body. The chancre lasts 3 to 6 weeks, and it heals without treatment. However, if adequate treatment is not administered, the infection progresses to the secondary stage. The characteristic rash of secondary syphilis may appear as rough, red, or reddish brown spots both on the palms of the hands and the bottoms of the feet. | Often asymptomatic. A painless open sore (chancre) appears between 10 days and 3 months after exposure. May also cause skin rash on hands and feet. All symptoms go away without treatment. | Direct contact with sores of infected person during vaginal, anal, or oral sex and from mother to child during childbirth. Case remains infectious for up to 2 years after infected. | Antibiotics | Can cause heart, brain, spinal cord, bone and joint damage. Can cause birth defects or miscarriage. Can cause death if untreated. | 36,000 new cases a year and increasing. | Slight - sores can exist in areas outside of condom coverage. |
| Trichomoniasis | Caused by a parasite. The vagina is the most common site of infection in women, and the urethra (urine canal) is the most common site of infection in men. | Usually asymptomatic in men, but could have irritation inside the penis, mild discharge, or slight burning after urniation or ejaculation. In women: vaginal discharge with strong odor, discomfort during intercourse and urination, irritation and itching of the female genital area. Rarely, lower abdominal pain. Symptoms appear within 5 to 28 days of exposure. | Penis-to-vagina intercourse or vulva-to-vulva (the genital area outside the vagina) contact with an infected partner. Women can acquire the disease from infected men or women, but men usually contract it only from infected women. | Metronidazole or tinidazole, given by mouth in a single dose. | Increase susceptibility to HIV. | 7.4 million new cases each year. | High |
| Genital Herpes (HSV) | Viral infection that causes blisters around the genitals, rectum, mouth or eyes. | Often asymptomatic. Blisters and open sores around the mouth or genitals/anus, flu-like symptoms including fever and swollen glands. Recurring outbreaks over lifetime. | Skin contact with infected area, with or without visible symptoms. It is possible to transmit an oral infection to the genitals and vice versa. | No cure. Antiviral medications shorten and prevent outbreaks. Daily suppressive therapy reduces transmission. | Painful sores, psychological distress, potentially fatal infections in babies, increased susceptibility to HIV. | 1 out of 5 adults has a genital HSV infection. | Slight - sores can exist in areas outside of condom coverage. |
| Human Papillomavirus (HPV) | The most common sexually transmitted infection. It affects the skin and mucous membranes and can cause genital warts, cervical dysplasia, and cancer of the cervix, vulva, perineum, anus, penis, and some skin, throat and oral cancers. | Usually asymptomatic. Warts causing strains can cause miniature cauliflower-like bumps in the affected area. HPV infections that have progressed to dysplasia will show pre-cancerous lesions. | Skin contact with infected area, with or without visible symptoms. Includes genital-to-genital contact, genital-to-anal contact, oral-to-genital contact, and hand-to-genital contact if the hands have not been washed thoroughly before touching uninfected genitals. | No cure. Vaccine for women prevents some transmission. Medications can remove warts. Cancer is treatable when detected. | HPV causes genital warts and cancer of the cervix, vulva, perineum, anus, penis, and some skin, throat and oral cancers. | The most common sexually transmitted infection. | Slight - infected areas can exist outside of condom coverage. |
| Hepatitus B | A virus that invades the liver and causes a contageous liver disease that can range in severity from mild illness lasting a few weeks to serious, lifelong illness. | Often asymptomatic. Jaundice, abdominal pain, loss of appetite, fatigue, joint pain, flu-like illness, nausea, vomiting, fever, dark urine. | Fluid transfer of infected blood, semen, vaginal fluid, or other body fluid. Sexual contact, sharing needles, and through childbirth. | There is no cure but a vaccine is available. | Can lead to liver cancer and liver failure. | 73,000 new infections every year. | Unknown |
| HIV/AIDS | A viral infection that destroys the immune system, leaving the body unable to fight off other infections. | Often asymptomatic for up to many years. Swollen glands, night sweats, weight loss. | Fluid transfer of infected blood, semen, vaginal fluid, or other body fluid. Sexual contact, sharing needles, and through childbirth. | There is no cure. Many treatments are available to prolong life and improve the quality of life. | This is a fatal disease. The virus destroys the immune system, leaving the body unable to fight off other infections. | 42,000 new infections every year. | 98% effective |
| Genital Lice (Crabs) | A parasite that feeds off the host and lives in the pubic region and other areas with coarse body hair, such as eyebrows, eyelashes, beard, mustache, chest, and armpits (but not on the head). | Persistent itch in pubic hair, usually worse at night. May see live crab or brown specks in underwear. | Contact with an infected person, especially sexual contact and possibly oral-to-genital contact if the crabs are present in facial hair (males and females). Also possible through sharing bedding, clothes, towels and possibly toilet seats. | Medicated lotion applied to pubic hair. | Secondary infections from scratching, social embarassment. | Unknown | Not effective. |
| Pelvic Inflammatory Disease | A serious infection in the uper genital tract/reproductive organs of a female. | Often asymptomatic. Lower abdominal pain, fever, unusual vaginal discharge, odor, painful intercourse, painful urination, irregular menstral bleeding, pain in the right upper abdomen. | Associated with gonorrhea and chlamydia. Intercourse, IUD contraceptives, and douching increase risk. | Antibiotics can cure PID but does not reverse any damage that has already occurred. | Can lead to infertility, ectopic pregnancy, abscess formation, and chronic pelvic pain. | 100,000,000 cases every year. | High |
| Pregnancy | While not a sexually transmitted disease or infection, it is a major sexual issue. | Morning sickness, missed period, increased weight gain, bloating, a fetus growing in the uterus. | Semenal fluid entering the vagina. | The Morning After pill, abortion, adoption, and birth. | Can lead to increased financial and emotional responsibility for a dependent for 18+ years. | Roughly 50% of pregnancies are unintended. | 98% effective. |
Sex is risky. But so is life in general. Everyone needs to determine what level of risk they are willing to take for themselves. But in open relationships, you can't be concerned only with yourself. When you have multiple intimate relationships, you have created a circle of people who love you and put their trust in you. The decisions you make affect everyone else. Remember the Poly Formula & Network Chart? That is a lot of people that you need to be responsible for.
You need to first decide what your level of acceptable risk is. Then, discuss with your partners and everyone in your group what level of acceptable risk and responsibility you are all willing to take for each other. How will new partners be introduced? How often will testing be done? Do you share your sexual history as part of your risk assessment? Do you discuss with potential partners to make sure everyone has the same definitions for "risk level" and that they have the same level of understanding as you for STDs?
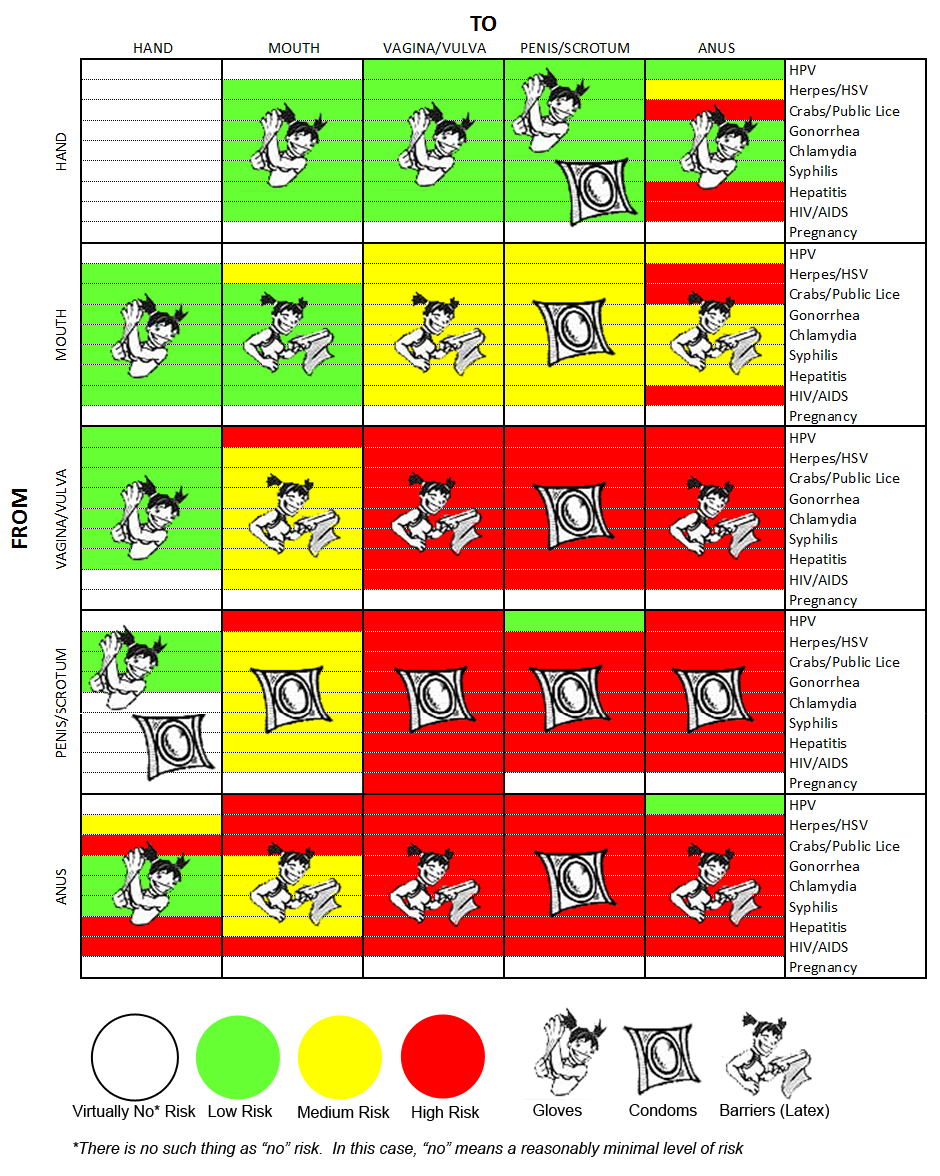
To help you decide what kinds of activities and boundaries to negotiate, check out this chart. Cute graphics are from www.methings.com and chart data gathered from LTA Sex and slightly modified to fit my version of the chart, which has the direction an STI would travel that LTA's chart does not.
It's tempting to just trust that the person you love will tell you all the information you need to know and has your best interests at heart. And that person might indeed believe they are telling you what you need to know and have your best interests at heart. But it is a fact that everyone has their own ideas about "what someone needs to know" and what someone's "best interests" are. When dealing with multiple sexual partners, the consequences are too high to simply rely on trust that your partners have the same definitions you do. This does not mean to imply that your partners are maliciously keeping secrets from you. This is a very realistic acknowledgment that we all come from different backgrounds and have our own assumptions and definitions about relationships. Clearly discussing your safe-sex requirements is merely one aspect of the "open and honest communication" that is so important in polyamorous relationships ... or in any relationship for that matter!
To that effect, I strongly recommend everyone keep a written list of sexual history, STD test dates, medical records, etc. And yes, I do mean literally, a written list (hand or typed or computer file) that you exchange for a written list with your potential partner(s). Again, this is not to imply your partners are lying. This is to provide a visual aid for clear communication, to make sure that you both have the same level of understanding of what each person means. I am a strong proponent of taking notes into a serious discussion to make sure you cover all the details you want to cover without accidentally forgetting something or leaving it out. I also advocate taking notes of the discussion, to ask for clarification later or to help remind you to make sure your assumptions and definitions are known and understood.
For an excellent guide to the kinds of information you may want to ask of your potential partners, download The Sexual Health & History Disclosure Form (you will need Adobe Acrobat to view this file). Yes, we actually fill it out and ask our partners to fill it out too. At one time, Google offered an internet-based service that let you keep track of all your health-related materials, forms, test results, x-rays, prescriptions, conditions, and medications that you can access from any computer with internet access (it was password-protected).
You could then connect accounts to the other people in your poly family (or any family, really), to more easily trade medial information among the relevant people. There was also an iPhone app that will let you access your account on your iPhone. Although Google discontinued that service, I highly recommend investing in and using a web-based medical service like Google Health for sharing important medical information. Think of it like sharing Google or iCal calendars with your poly family, only instead of dates, it's test results and medication information.
Open and honest communication, with regards to health issues, results in significantly fewer medical complications, even with more partners. This has been shown to be both statistically true and practically true, as studied among populations with multiple partners. The more open the communication about health, the more healthy the population is as a whole.
The Inn Between © 2002
Contact The InnKeeper